Doctors had little hope for a fetus with a fatal lung condition, but at his parents’ urging, they performed an unprecedentedly early operation during which they partially removed him from the womb.
The procedure saved the child’s life — baby Cassian was born in August 2025 and is still doing well. The doctors hope the same approach will save others in the future.
The diagnosis came during a second-trimester ultrasound at Orlando Health Winnie Palmer Hospital for Women & Babies in Florida. The scan revealed overinflated lungs and a compressed heart — signs of a dangerous condition called congenital high airway obstruction syndrome (CHAOS).
A risky strategy
A scope revealed that the blockage in Cassian’s widepipe was a 0.2-inch-thick (5 millimeters) membrane, which was too large to puncture using a minimally invasive laser probe.
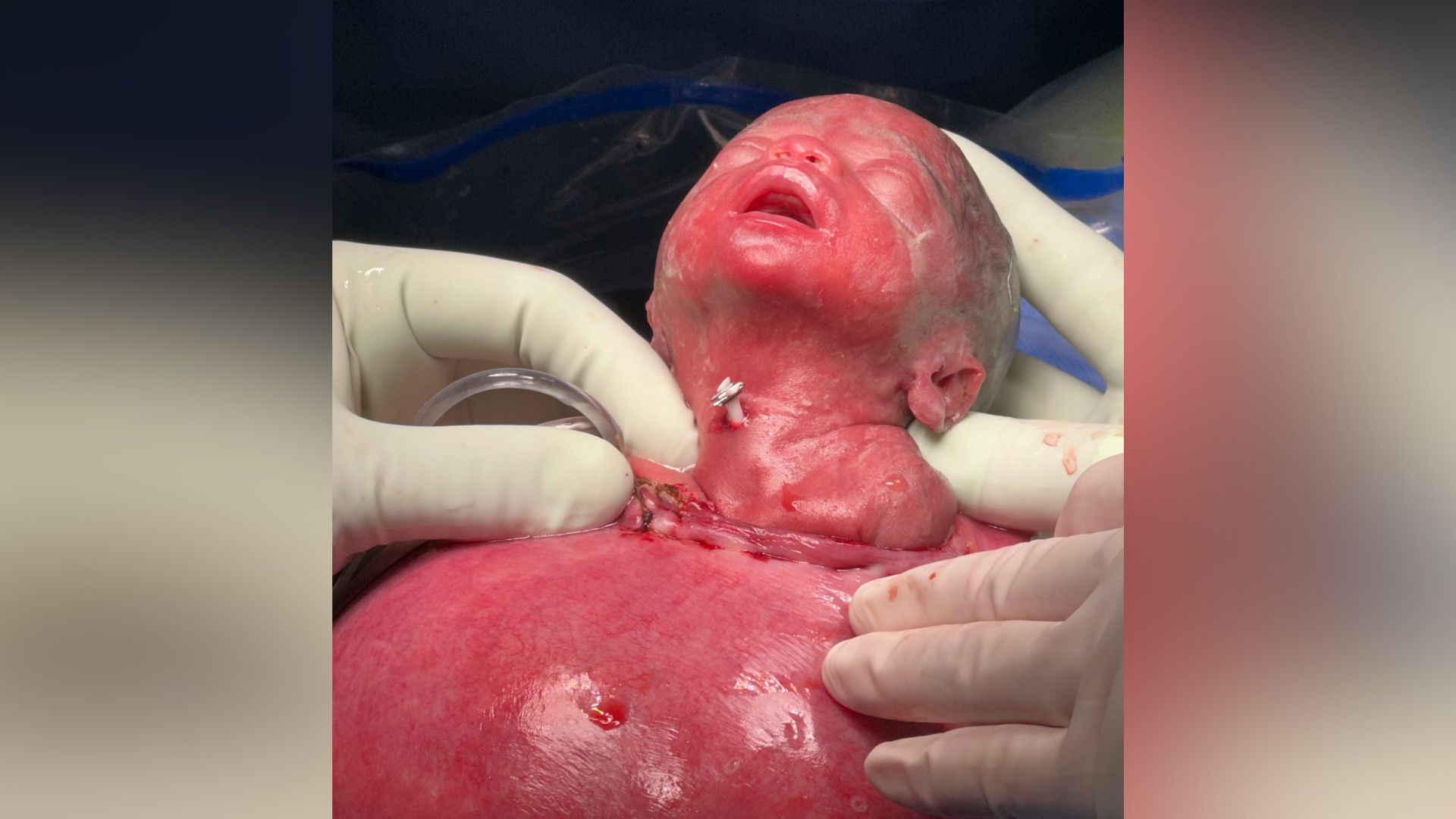
Doctors have a method for safely delivering babies with these types of airway obstructions. Ideally, they wait until weeks 37 to 39 of pregnancy before using a variant of a cesarean section that involves delivering the head, neck and shoulders of the fetus first while the lower body remains in the womb. At this point, the baby is effectively half born.
Doctors then insert a catheter to bypass the blockage, drain the fluid and allow the baby to breathe, before clamping the umbilical cord and delivering the baby completely. This procedure, called the ex-utero intrapartum treatment (ExIT), is routinely performed on patients with CHAOS.
However, 1 in 4 fetuses with CHAOS die of heart failure before reaching those final weeks of pregnancy, said Dr. Emanuel Vlastos, another one of Cassian’s fetal surgeons. This scenario seemed probable for Cassian, whose heart couldn’t grow properly under the pressure of his distended lungs.
Cassian’s parents urged doctors to try anything they could, leading the medical team to propose a potentially risky operation. At just 25 weeks, they would perform the ExIT, drain Cassian’s lungs of fluid before his heart condition worsened, and place him back in the womb to continue developing.
“When you hear the parents say something to the effect of, ‘Well, we know this may not work out, but if you can learn something and help another child, it’s probably going to be worthwhile’ — that’s a pretty magnanimous thing for a parent to say, knowing their baby may die,” Vlastos said.
With permission from an ethics committee, the surgeons operated on Cassian and his mother Kieshera at 25 weeks of pregnancy. This involved conducting a C-section to expose Cassian’s head and neck and then inserting a catheter into his windpipe to drain his lung secretions. Then, they returned his upper body into the womb and closed it. The catheter remained, held firmly in place by an inflated balloon in his windpipe, for the remainder of the pregnancy.
Given that the ExIT is typically performed at the time of child birth, this may be the first time doctors inserted a windpipe catheter into a fetus this early in gestation and returned him to the uterus, Greves said.
Balancing two lives
Operating on a fetus requires factoring in the mother’s health, too.
“It is a tightrope walk, sometimes for several hours, while two lives hang in the balance,” Greves said.
In this case, the team used general anesthesia to sedate mother and child, but doctors aren’t sure what effects general anesthesia has on the developing nervous system of a 25-week fetus, Vlastos noted. Some studies suggest anesthesia can disrupt the formation of links between nerve cells and lead to cognitive issues, for example.
But it was imperative to sedate the fetus so he wouldn’t attempt to breathe once exposed to air. “There’s a whole lot of circulatory changes that potentially could happen if the baby tried to breathe,” Vlastos said. And those changes could make it impossible to carry out the rest of the pregnancy.
Fetuses receive oxygen via the placenta rather than by breathing themselves; in the womb, a blood vessel called the ductus arteriosus forces oxygenated blood to bypass the immature lungs and directs it to the rest of the fetal body. “Once kids start to breathe outside of the womb, that vessel begins to slowly close” so that blood can travel to the lungs to pick up oxygen, Vlastos said. The doctors would not have been able to return Cassian to the womb if he had begun breathing.
They never stopped asking the very important question, “What else could we try?”
Dr. Cole Greves, one of Cassian’s surgeons at Orlando Health Winnie Palmer Hospital for Women & Babies
For Cassian’s mother Kieshera, general anesthesia ensured that her uterine muscles relaxed during the procedure. Otherwise, “the baby’s going to erupt” and be delivered early, Vlastos said, as the uterus is prone to contract when incised. What’s more, a surgically opened uterus can expel a lot of blood if it starts contracting, leading to a potentially dangerous hemorrhage for the mother.
Another concern with operating on a preterm fetus is disrupting the delicate process of development. For example, if the balloon that held the catheter in place were underinflated, the catheter could have slid down and put pressure on the windpipe, preventing it from developing, Vlastos said. And if it were overinflated, the balloon could compress the blood vessels draining the head, causing circulatory issues, he added.
Inflating a balloon in the widepipe could pose a number of concerns, Dr. Diana Farmer, a fetal surgeon at the University of California, Davis Health who was not involved in this case, told Live Science in an email.
But “I like to say ‘there’s a lot we can do for a live patient,'” she said. “And the tracheal issues can be dealt with after birth.”
The outcome
At week 31 of pregnancy, six weeks out from the daring surgery, Kieshera’s uterus started contracting and the time came to deliver baby Cassian. Scarring from the earlier surgery may have made her more likely to go into labor early.
A team of 30 people assembled at 3 a.m. to perform an ExIT, as had been planned, Vlastos said.
The team exposed Cassian’s head and neck and swapped the fluid-draining catheter in the windpipe for an intubation tube to help the newborn breathe. He was born relatively healthy, although he needed to remain in the hospital for a few months due to being born prematurely.
Today, Cassian remains on a ventilator but is being weaned off respiratory support. When he’s older, he’ll require surgery to clear the obstruction in his windpipe and allow his breathing tube to be removed for good.
Cassian’s story shows that this early intervention can work, fostering hope for other CHAOS cases.
“This work would best be carried out in the context of a clinical trial with rigorous data collected on the development impacts of the lung and tracheal growth,” Farmer said. “But these are difficult to accomplish in rare diseases.”
Vlastos said fetal surgeons, globally, should come together to discuss whether they have performed similar operations and to think of new strategies to improve the surgery. For instance, they could find smaller catheters that are more appropriate for a fetus or develop less invasive approaches to drain the lungs.
Cassian’s surgery may sow the seeds for doctors to perform similar operations in the future, but it would never have happened if it weren’t for the trust of his parents.
“They never stopped asking the very important question, ‘What else could we try?'” Greves said. “I do believe, in the end, this made all the difference.”
This article is for informational purposes only and is not meant to offer medical advice.